
ResultsĮighty-one infants with a median (range) gestational age of 28.7 (22.4–41.9) weeks were recruited. Alveolar ventilation ( V A) was also calculated. Volumetric capnograms were constructed to calculate the dead space using the modified Bohr–Enghoff equation. Expiratory tidal volume and carbon dioxide levels were measured. MethodsĪ prospective study of mechanically ventilated infants was undertaken. We determined if there were differences in dead space and alveolar ventilation in ventilated infants with pulmonary disease or no respiratory morbidity. A significant association of DS with both death (HR 1.204 CI 1.019–1.423 p = 0.029) and discharge (HR 0.434 CI 0.414–0.456 p \(< 0.001\)) was noticed even when correcting for confounding factors (age, sex, chronic obstructive pulmonary disease, diabetes, PaO \(_\) ratio), is easy to collect and focuses on physiological quantities directly measured from the patient.Dead space is the volume not taking part in gas exchange and, if increased, could affect alveolar ventilation if there is too low a delivered volume. The final population consisted of 401 patients from seven ICUs. 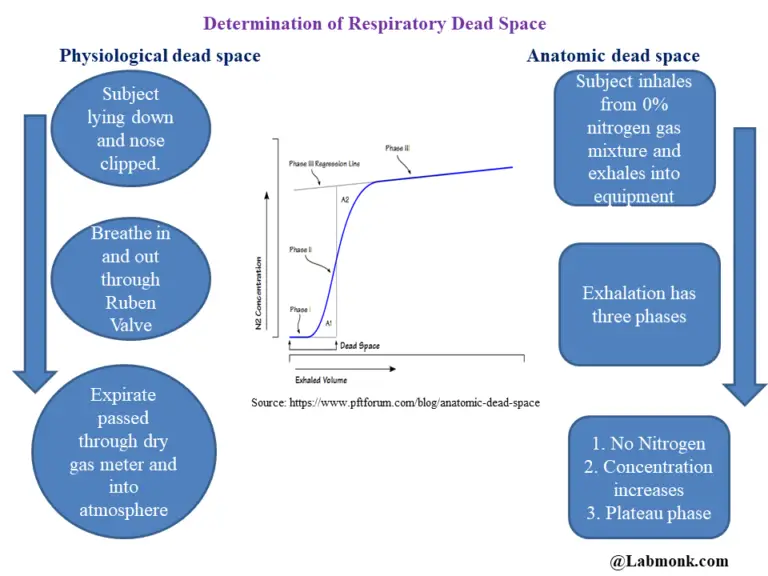 
A competing risk Cox proportional hazard model was applied to test for the association of DS with two competing outcomes (death or discharge from the ICU) while adjusting for confounders. Retrospective cohort study on data derived from Italian ICUs during the first year of the COVID-19 epidemic. Here, we explore the association between a surrogate measure of dead space (DS) and early outcomes of mechanically ventilated patients admitted to Intensive Care Unit (ICU) because of COVID-19-associated ARDS. Physiologic dead space is a well-established independent predictor of death in patients with acute respiratory distress syndrome (ARDS).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
